Willkommen bei DELTA meditec Ihrem Partner in der Medizintechnik.
Wir bieten Ihnen das `Rundum-Paket`: Beratung, Vertrieb und Service. Alles individuell auf Sie zugeschnitten.
Egal ob Klinik, Arztpraxis oder Physiotherapiepraxis DELTA meditec bieten Ihnen eine große Auswahl an neuen und gebrauchten Diagnose- und Therapiegeräten. Wir bieten Ihnen kompetenten Service und eine Reihe attraktiver Leistungen rund um Kundendienst und Reparatur.
Unsere Angebote
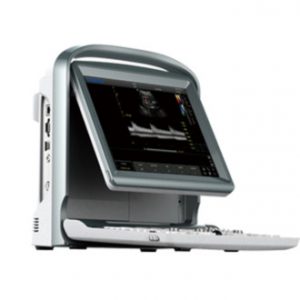
CHISON ECO5 – für nur 8.999€
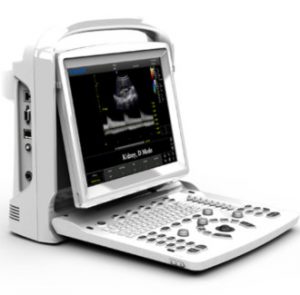
CHISON ECO3 Expert -für nur 6.999€
Tragbares s/w Ultraschallsystem mit PW-Doppler
Weitere Ultraschallgeräte
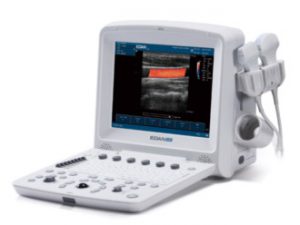
Edan U50 Prime -für nur 7.999€
Edan SE-1200 – für nur 1.650€
24 Stunden Reparatur-Service
Wir lassen Sie nicht im Stich!